Therapeutic pipeline
From overlooked insights to outsized value for kidney patients
Our process has cultivated an impactful biotech system, geared towards bringing innovative solutions to market for a wide range of unmet patient needs. Currently, our pipeline includes assets covering a full spectrum of kidney disease concerns.
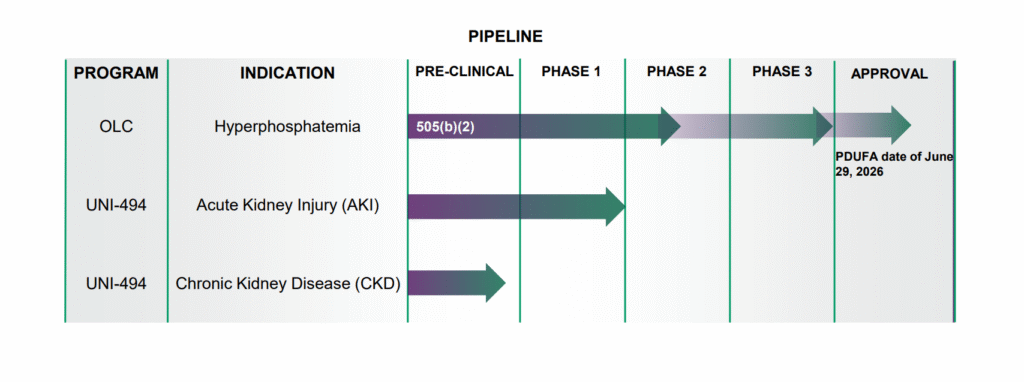
OLC has received a PDUFA date of June 29, 2026 from the FDA.
Oxylanthanum Carbonate (OLC)
Oxylanthanum carbonate (OLC) is a next-generation lanthanum-based phosphate binding agent utilizing proprietary nanoparticle technology being developed for the treatment of hyperphosphatemia in patients with chronic kidney disease (CKD). OLC has over forty issued and granted patents globally. Its potential best-in-class profile may have meaningful patient adherence benefits over currently available treatment options as it lowers the pill burden for patients in terms of number and size of pills per dose that are swallowed instead of chewed.1
OLC has received a PDUFA date of June 29, 2026 from the FDA.
UNI-494
UNI-494 is a novel nicotinamide ester derivative and a selective ATP-sensitive mitochondrial potassium channel activator. UNI-494 has a novel mechanism of action that restores mitochondrial function and may be beneficial for the treatment of several diseases including Acute Kidney Injury (AKI).
If approved, UNI-494 would be the first and only available therapy for treating AKI.